Trauma-Informed Care: What It Means and Why It Matters in Functional Medicine
What does it mean to be trauma-informed—and why is trauma-informed care essential for healing?
Trauma-informed care refers to an approach used in healthcare, mental health, education, and clinical programs that recognizes the widespread impact of trauma and integrates that awareness into every interaction, policy, and environment.
It’s not a specific therapy or technique.
It’s a framework and clinical mindset that shapes how care is delivered.

What Is Trauma-Informed Care? (Core Definition)
A trauma-informed approach assumes that many individuals have experienced trauma, understands how trauma affects the brain and behavior, and responds in ways that promote:
- Safety
- Trust
- Empowerment
—all while actively avoiding re-traumatization.
What Counts as Trauma?
Trauma is not limited to extreme or catastrophic events. It includes a wide range of experiences that impact the nervous system, such as:
- Emotional, physical, or sexual abuse
- Neglect or attachment disruption
- Chronic stress (illness, poverty, racism, medical trauma)
- Loss, grief, or betrayal
- Adverse Childhood Experiences (ACEs)
Clinically, trauma often presents as nervous system dysregulation, not just psychological distress.
The 6 Principles of Trauma-Informed Care
Trauma-informed systems are built on six foundational principles:
1. Safety
- Prioritizes physical, emotional, and psychological safety
- Creates a calm, predictable, and non-threatening environment
2. Trustworthiness & Transparency
- Clear expectations with no surprises
- Open, honest communication
3. Peer Support
- Encourages connection with others who have lived experience
- Reduces isolation and shame
4. Collaboration & Mutuality
- Shared decision-making
- “We do this with you, not to you”
5. Empowerment, Voice & Choice
- Patients have agency and autonomy
- Individual pacing, preferences, and goals are respected
6. Cultural, Historical & Gender Awareness
- Recognizes systemic and identity-based trauma
- Avoids one-size-fits-all care
What Trauma-Informed Care Looks Like in Practice
In a Trauma-Informed Clinician
A trauma-informed clinician:
- Asks: “What happened to you?” instead of “What’s wrong with you?”
- Recognizes signs of nervous system dysregulation (fight, flight, freeze, fawn)
- Avoids shame, blame, or minimization
- Offers choice and consent in care
- Practices self-regulation to support co-regulation
In a Trauma-Informed Program
A trauma-informed program:
- Uses intake processes that avoid triggering language
- Clearly explains what patients can expect
- Allows flexibility in pacing (no forced compliance)
- Trains staff in trauma awareness and de-escalation
- Designs environments that reduce sensory overwhelm (lighting, noise, etc.)
What Trauma-Informed Care Is NOT
It’s important to clarify what trauma-informed care is not:
- It is not just being nice or empathetic
- It does not avoid difficult conversations
- It is not a specific modality like CBT, EMDR, or somatic therapy
Instead, it is the foundation (or container) in which all therapeutic approaches are delivered.
Why Trauma-Informed Care Matters (Clinical Perspective)
Trauma has measurable effects on the body and brain, including:
- Neurobiology (amygdala hyperreactivity, reduced prefrontal regulation)
- Autonomic nervous system dysfunction
- Hormonal imbalance (HPA axis dysregulation)
- Immune activation and chronic inflammation
Without a trauma-informed approach, care may unintentionally:
- Trigger shutdown or resistance
- Reinforce shame
- Lead to poor adherence or treatment drop-out
Trauma-Informed Care in Functional Medicine & Psychiatry
From a functional medicine and functional psychiatry perspective, trauma-informed care is essential.
Trauma is often a root contributor to:
- Chronic inflammation
- Gut dysbiosis
- HPA axis dysfunction
- Sleep disturbances
It also directly impacts:
- A patient’s ability to follow nutrition and lifestyle protocols
- Tolerance to detoxification and treatment intensity
Key Insight:
You can have the perfect treatment plan—but if the nervous system does not feel safe, the body cannot fully receive or implement it.
A Simple Clinical Reframe
Instead of asking:
“Why isn’t this patient following the plan?”
Ask:
“What is their nervous system protecting them from right now?”
Bottom Line: What Defines a Trauma-Informed Program?
A truly trauma-informed approach:
- Prioritizes safety and nervous system regulation
- Builds trust through transparency
- Shares power and supports collaboration
- Honors patient autonomy and pacing
- Understands symptoms as adaptations—not pathology
Start Your Healing with a Trauma-Informed Approach
At Functional Mind, we specialize in trauma-informed care within a functional medicine and psychiatry framework—addressing the root causes of mental and physical health concerns while honoring your nervous system, pace, and lived experience.
If you’re ready for a personalized, compassionate approach to healing, we invite you to take the next step.
📞 Call us at 401-270-4541
🗓️ Book your Discovery Call: https://fxnmind.com/free-consultation-with-achina/
Your healing journey deserves a space that feels safe, collaborative, and truly supportive.












 Most people think of brushing and flossing as basic daily habits to prevent cavities — but your oral health influences far more than your smile. Strong research now shows a significant link between oral health and brain health, revealing that the state of your mouth directly affects cognitive function, inflammation, and long-term brain wellness.
Most people think of brushing and flossing as basic daily habits to prevent cavities — but your oral health influences far more than your smile. Strong research now shows a significant link between oral health and brain health, revealing that the state of your mouth directly affects cognitive function, inflammation, and long-term brain wellness.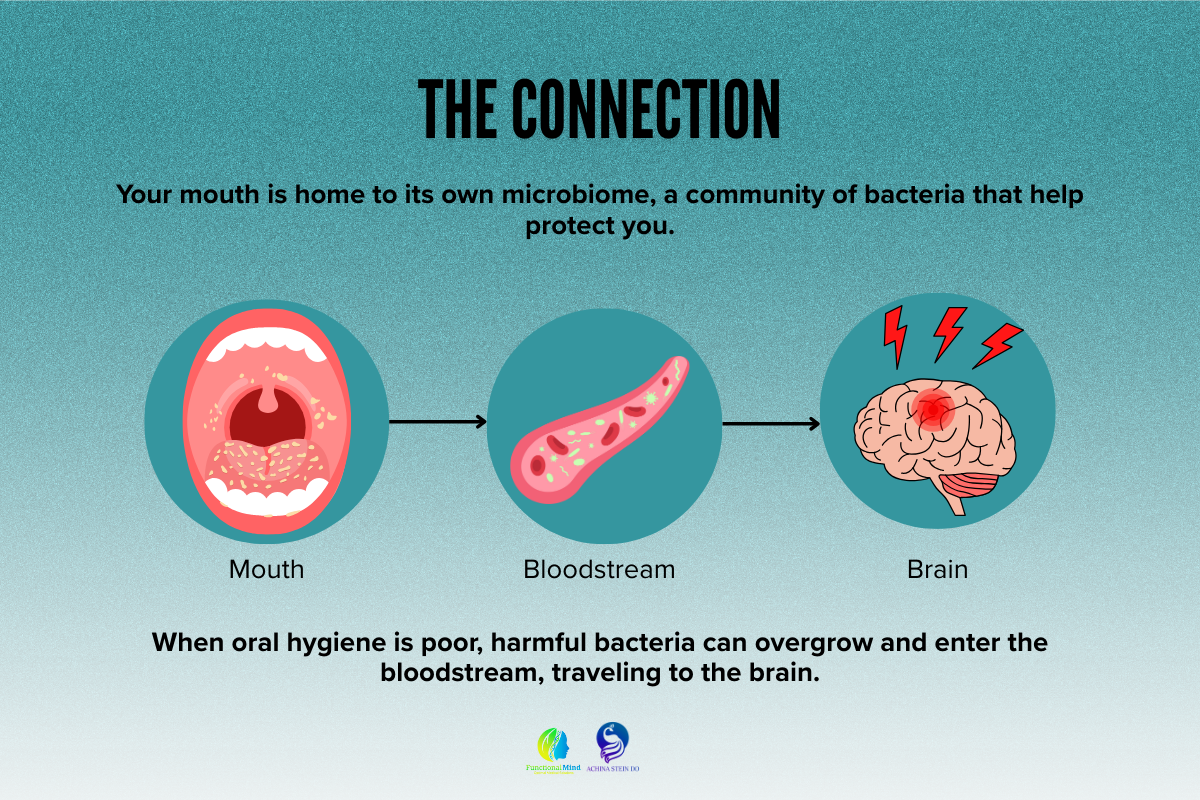 Your mouth contains millions of bacteria. Some are helpful, but others can trigger inflammation when they grow out of balance. When harmful bacteria flourish due to gum disease, poor hygiene, or unresolved dental issues, they can enter the bloodstream and travel to the brain.
Your mouth contains millions of bacteria. Some are helpful, but others can trigger inflammation when they grow out of balance. When harmful bacteria flourish due to gum disease, poor hygiene, or unresolved dental issues, they can enter the bloodstream and travel to the brain.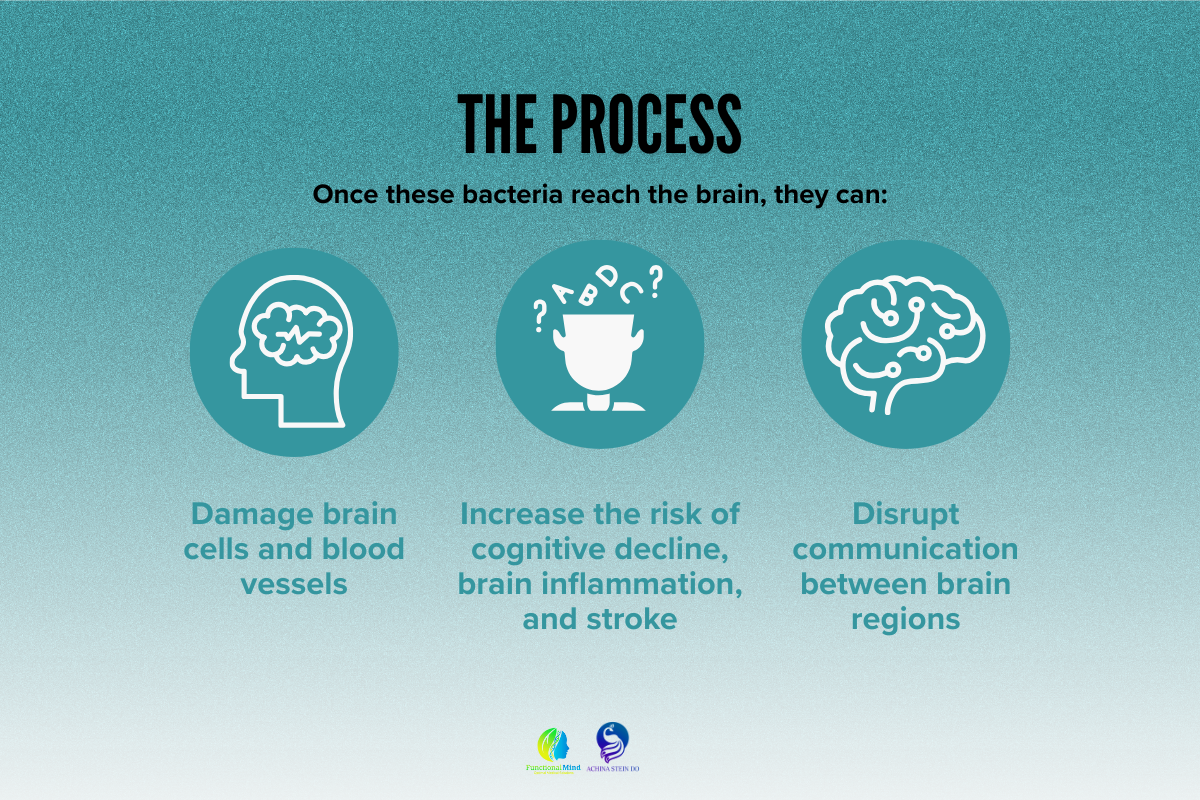
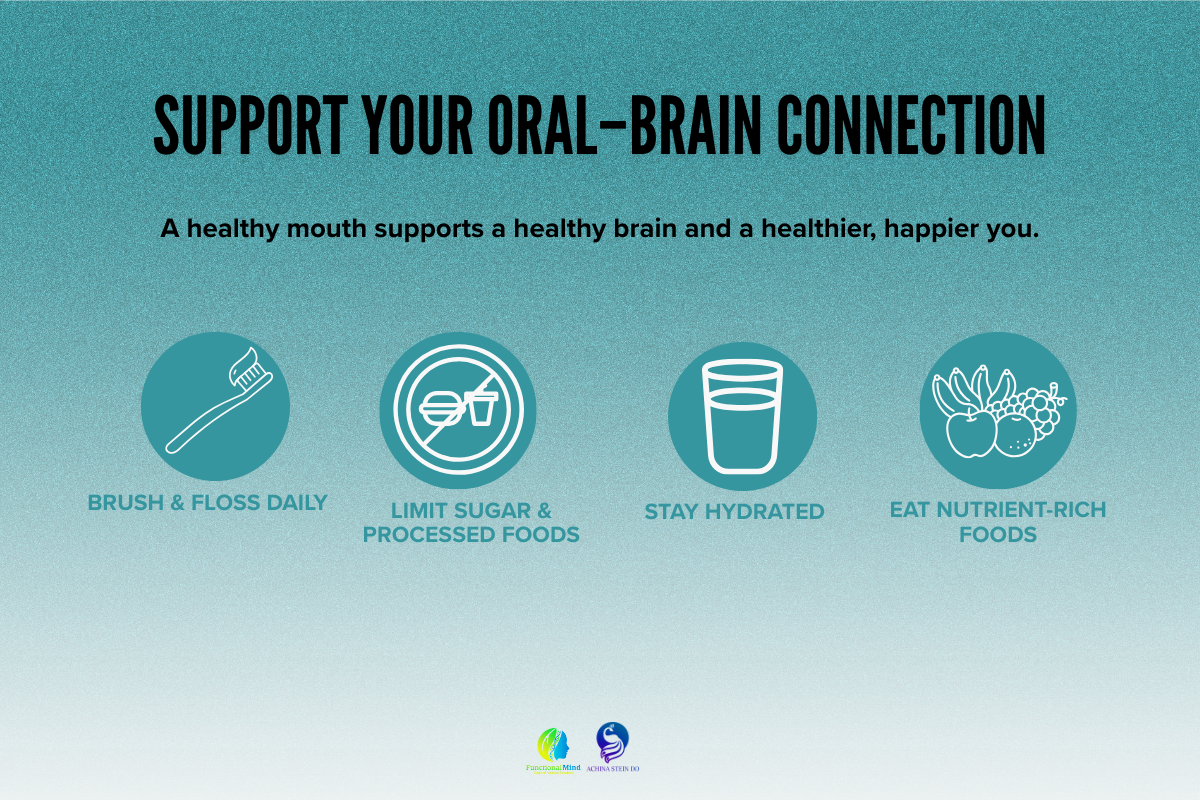 Improving your mouth is one of the most effective ways to protect your brain. Here are key steps:
Improving your mouth is one of the most effective ways to protect your brain. Here are key steps: Heart Rate Variability measures the slight variations in time between each heartbeat. Even if your heart beats 70 times per minute, the spacing between beats isn’t perfectly even — and that variability is healthy.
Heart Rate Variability measures the slight variations in time between each heartbeat. Even if your heart beats 70 times per minute, the spacing between beats isn’t perfectly even — and that variability is healthy.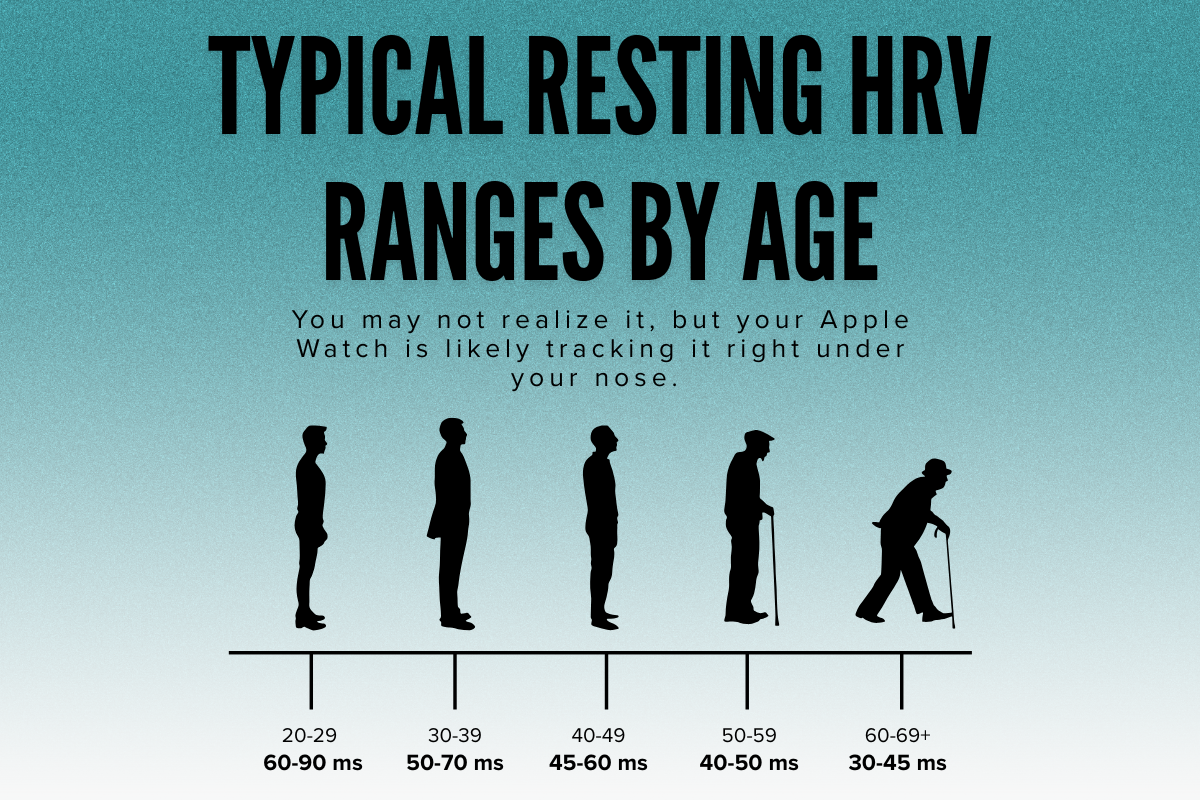 HRV varies from person to person, but here are general resting HRV ranges:
HRV varies from person to person, but here are general resting HRV ranges: HRV is closely connected to emotional balance and mental resilience. Low HRV is associated with:
HRV is closely connected to emotional balance and mental resilience. Low HRV is associated with: You can raise your HRV and strengthen your stress resilience with simple daily habits:
You can raise your HRV and strengthen your stress resilience with simple daily habits: